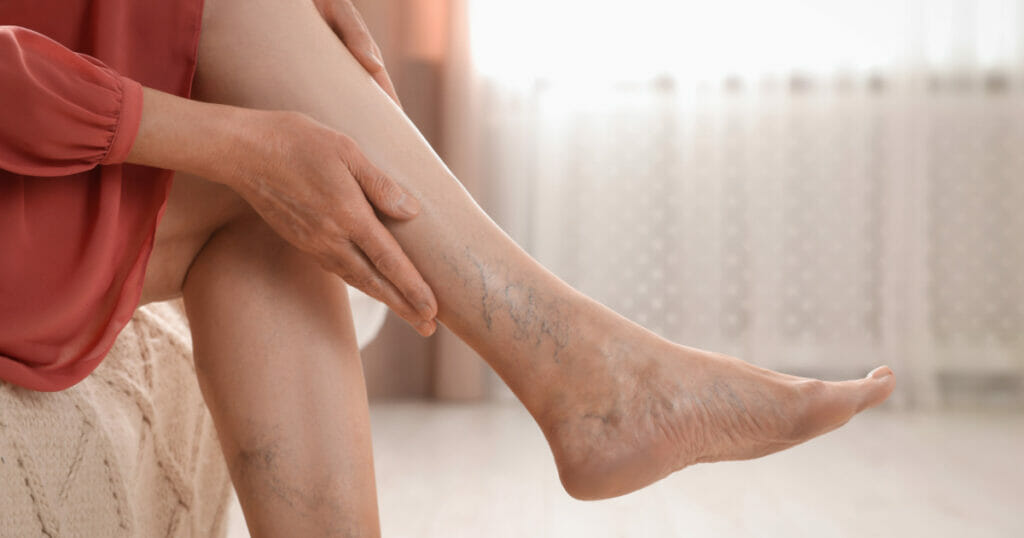
If you’ve noticed tiny, threadlike red or blue veins on your legs, ankles, or feet that resemble a spider web, then you likely have spider veins. While many of us are familiar with these harmless cosmetic blemishes, what about varicose veins?
Varicose veins can appear similar to spider veins in color and size but they are very different things. To better understand the differences between varicose vein vs. spider vein, it is important to consider their distinctive features so that treatments can be tailored for each condition accordingly.
In this blog post, we will explore the key ways in which both of these common vascular conditions differ as well as when to seek professional medical care.
What are Varicose Veins?
Varicose veins are a prevalent medical condition that can manifest in various areas of the body, with the legs being a common location. They primarily stem from impaired blood circulation within the veins, leading to the abnormal enlargement, twisting, and protrusion of these blood vessels.
Varicose veins exhibit a wide spectrum of sizes, spanning from minor to substantially large. When large varicose veins develop, they exert added stress on adjacent healthy veins, potentially compromising overall vein function and health. In certain instances, this condition may escalate to the formation of blood clots, a critical medical concern that warrants prompt attention.
What are Spider Veins?
Spider veins, also known as telangiectasia, are small, dilated blood vessels that appear near the surface of the skin. They often manifest as red or purple lines and web-like patterns, typically found on the legs and face. Spider veins are generally harmless but can be unsightly and may cause discomfort in some cases.
These veins occur when there is an increase in pressure within the blood vessels, causing them to become enlarged and visible. The exact cause of spider veins is not fully understood, but they can be influenced by factors such as genetics, hormonal changes, pregnancy, obesity, prolonged standing or sitting, and sun exposure.
[Related: Sclerotherapy for Varicose Veins: How Does It Work?]
Varicose Vein Causes and Symptoms
Varicose veins are enlarged and twisted veins that commonly appear in the legs. These bothersome leg veins can be caused by various factors, including:
- Weak or damaged valves: Inside the veins, there are tiny valves that help regulate blood flow. If these valves become weak or damaged, blood can pool in the veins, causing them to enlarge and become varicose.
- Increased pressure on the veins: Prolonged standing or sitting can put increased pressure on the veins in the legs, leading to the development of varicose veins.
- Hormonal changes: Changes in hormone levels, such as those that occur during pregnancy or menopause, can relax the vein walls and contribute to the formation of varicose veins.
- Family history: There is often a genetic component to varicose veins. If your parents or close relatives have them, you are more likely to develop them as well.
- Obesity: Excess weight can put added pressure on the veins, increasing the risk of developing varicose veins.
- Age: The risk of varicose veins increases with age, as the veins may lose elasticity and become weakened over time.
Symptoms of varicose veins can vary from person to person, but commonly include:
- Bulging veins
- Aching and heaviness in the legs
- Swelling in the affected area
- Itching
- Leg cramps
- Restless legs syndrome
- Skin changes (discoloration, dryness, irritation)
- Development of open sores or ulcers, usually near the ankles.
Spider Veins Causes and Symptoms
The causes of spider veins can include:
- Heredity: A family history of spider veins can increase the likelihood of developing them.
- Prolonged standing or sitting: Occupations that involve long periods of standing or sitting can contribute to the development of spider veins.
- Hormonal changes: Pregnancy, menopause, and the use of hormonal birth control can lead to the development of spider veins.
- Obesity: Excess weight puts added pressure on the veins, increasing the risk of spider veins.
- Trauma or injury: Previous injuries or trauma to the skin can cause damage to blood vessels and contribute to the formation of spider veins.
- Medical conditions: Certain medical conditions like liver disease or blood clotting disorders can increase the risk of developing spider veins.
- Age: The risk of spider veins tends to increase with age as the veins lose elasticity.
- Sun exposure: Prolonged exposure to the sun’s harmful UV rays can weaken the skin and blood vessels, leading to the appearance of spider veins.
[Related: 9 Things to Ask Your Varicose Vein Doctor About Your Treatment]
What Are the Ways to Treat Varicose Veins?
If you’re dealing with varicose veins or spider veins, you may feel self-conscious or uncomfortable. Fortunately, there are various treatments available to help. In this section, we’ll explain the treatment options for both varicose veins and spider veins.
Varicose Vein Treatment
Treatments for varicose veins range from minimally invasive procedures to surgery. Non-invasive procedures include:
- Endovenous laser treatment: This minimally invasive treatment uses a laser to close off the affected veins, rerouting blood flow to healthy veins.
- Sclerotherapy: A solution is injected into the affected veins, causing them to collapse and eventually be reabsorbed by the body.
- Radiofrequency ablation: This procedure uses radiofrequency energy to heat the walls inside the damaged vein and close it.
If you have severe varicose veins, our doctors may recommend surgery. Common surgical procedures for varicose veins include:
- Vein stripping: This involves removing the affected veins through incisions in the skin.
- Ambulatory phlebectomy: This procedure involves making small incisions in the skin and using a hook to remove the affected veins.
Spider Veins Treatment
Minimally invasive procedures can be used to treat spider veins, including:
- Laser treatments: This procedure uses a laser to target and close off the affected veins.
- Sclerotherapy: This is a minimally invasive procedure in which a solution is injected into varicose or spider veins to cause them to collapse and fade from view.
It’s important to note that while these treatments can be effective, they don’t prevent new spider veins from forming. Our doctors may recommend additional treatments or steps to help prevent new spider veins from appearing.
Prevention Techniques for Varicose Veins and Spider Veins

Preventing varicose veins and spider veins involves making some lifestyle changes. Here are some of the prevention techniques we recommend:
- Wear Compression Stockings: Compression stockings are an effective way to reduce the risk of varicose veins and spider veins. They help improve blood flow, prevent blood from pooling in your legs, and reduce swelling. These stockings are available in different sizes and compression levels. Consult your doctor to determine the best one for you.
- Maintain a Healthy Weight: Being overweight or obese puts extra pressure on your veins, which can lead to varicose veins and spider veins. Maintaining a healthy weight through a balanced diet and regular exercise can help prevent these conditions.
- Stay Active: Engage in regular physical activity to improve blood flow in your legs. Low-impact exercises such as walking, swimming, and cycling can help improve circulation.
- Elevate Your Legs: Elevating your legs above heart level can help reduce swelling and pressure on your veins. Try elevating your legs for a few minutes every day.
- Avoid Prolonged Sitting or Standing: Prolonged sitting or standing can put extra pressure on your legs and lead to varicose veins and spider veins. Take breaks to stretch and move your legs throughout the day.
- Avoid Tight Clothing: Tight clothing, especially around your waist, groin, and legs, can restrict blood flow and increase the risk of varicose veins and spider veins.
Get High-Quality Vein Care
To sum up, varicose veins and spider veins can look very similar, yet they’re quite distinct. If you suspect that you may have either varicose or spider veins, do not hesitate to set an appointment with us today!
Our team is composed of board-certified specialists who remain vigilantly up-to-date on the latest advancements in venous medicine and have extensive experience in treating both types of vein conditions.
Set an appointment with us today!
Vascular & Interventional Specialists of Prescott was formed in 2010 by a group of subspecialty radiologists that perform numerous minimally-invasive, low-risk procedures using the tools of our trade for guidance—x-ray, ultrasound, CT scan, and MRI. The team’s goal is to educate patients and medical communities, while also providing safe and compassionate health care, with rapid recovery times and low risk of complications.
