Varicose Veins
What Are Varicose Veins?
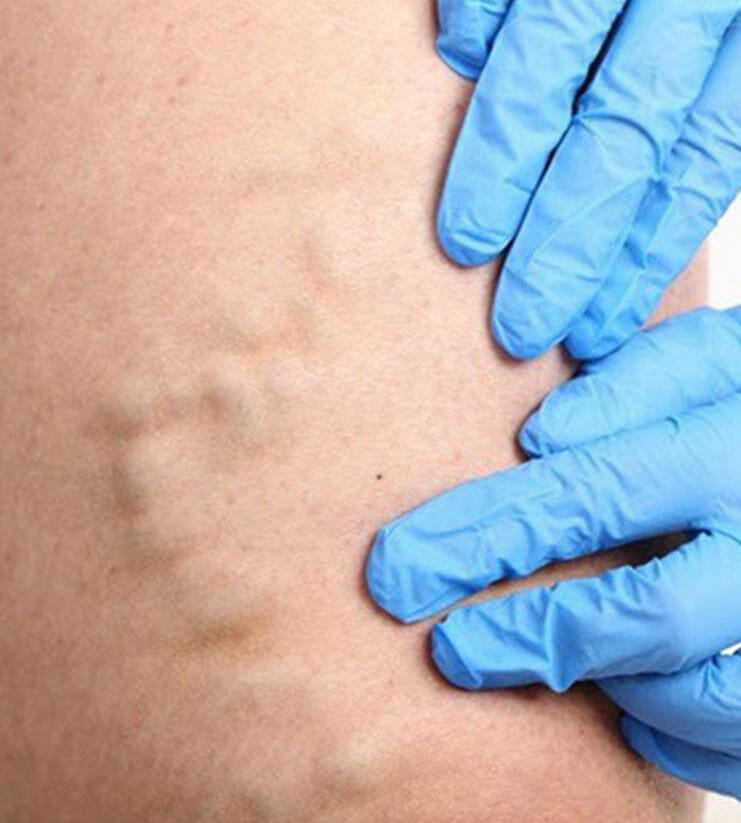
Varicose veins are large swollen veins that appear just below the surface of your skin. They develop when blood from your extremities (usually your feet) doesn’t flow effectively through your veins. This causes the veins in your legs to widen and bulge as the blood pools. Generally, the varicosity of veins is not a cause for an emergency. However, since they don’t look good, a lot of people get these bulging veins removed. In addition, some cases like those with swelling, aching, or painful veins are recommended to undergo medical treatment, as these can be signs of serious medical conditions.
Symptoms of Varicose Veins
Symptoms vary from person to person but usually include:
- Heavy feeling in the legs
- Burning or aching sensation in the legs
- Skin color changes
- Rash
- Sores on the legs
Common Causes of Varicose Veins
Blood from the lungs travels through your arteries and delivers oxygen to the different parts of your body. Subsequently, blood then gets propelled back to your heart through your veins. These veins operate on a network of one-way valves. To prevent backflow, these cup-like valves alternately open to allow blood to flow towards the heart. For people with varicose veins, these valves aren’t functioning well. Thus, blood pools and exerts extra pressure on the vein. This causes the vein to bulge and twist.
Conditions that put more pressure on your abdomen or legs make you more likely to have varicose veins:
- Gender. Females release hormones that relax veins. Those who are taking birth control pills or hormonal therapies are at greater risk.
- Being overweight or obese. Carrying extra weight can make it more difficult for your veins to flow blood properly.
- Family history. Genetics plays a role in increasing your risks as well. It is common for people with a history of vascular disease to pass it on to their children.
- Age. Veins go through wear and tear as you get older.
- Work that requires standing up too long. Jobs that demand you to sit or stand for long periods can increase your chances of having varicose veins.
- Pregnancy. It happens often to pregnant women due to hormonal changes and increased blood volume.
Varicose and Spider Veins – Is there a Difference?
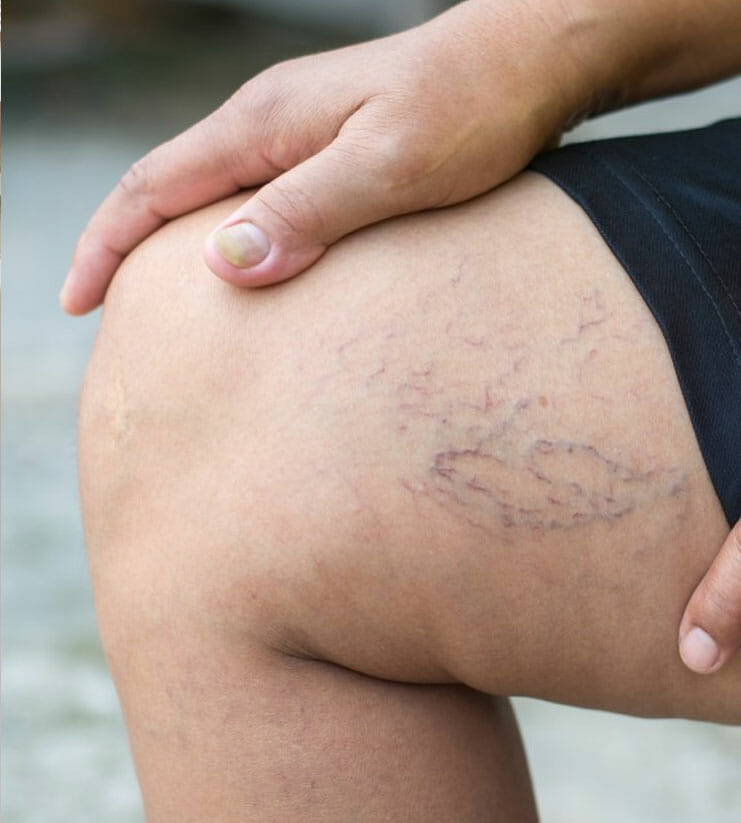
Although both are considered vein disorders, varicose and spider veins differ in certain ways:
- Spider Veins. Look like tiny, thin, web-like veins on the surface of the skin. Often, they appear almost like a bruise (reddish or purple colored). Commonly, they do not cause problems and are primarily treated to improve appearance.
- Varicose Veins. Present as larger and bulging veins under the skin. They usually appear green or blue. Treatments are generally done to provide relief and comfort for those experiencing related aches and pains.
How to Get Rid of Varicose Veins Naturally
If your varicose veins aren’t causing you pain, there are easy at-home remedies you can do to improve its appearance. In addition, following these tips can prevent varicose veins from getting worse.
5 Easy At-home Remedies For Varicose Veins
- Use compression stockings. These special stockings improve blood flow in the feet and legs. They are tighter at the ankle and get looser going up the knees.
- Avoid walking in high heels and wearing tight clothing around the thighs or waist.
- Reduce salt intake. Limiting your consumption of salty foods can help decrease swelling in the lower extremities.
- Achieve your ideal weight. Good nutrition and regular exercise can help you drop the extra pounds.
- Be conscious of how you sit and rest. Avoid crossing your legs when sitting. You can also prop your feet when sitting or sleeping.
The Best Treatment for Varicose Veins
Professional Treatments
Here at Vascular & Interventional Specialists of Prescott (VISP), we provide the best professional treatment for varicose veins. We offer:
- Ambulatory Phlebectomy. A minimally invasive procedure, the ambulatory phlebectomy is the removal of the vein through small slit-like incisions.
- Injection Sclerotherapy. This is used to treat smaller varicose and nearly all spider veins to provide pain relief and improve their appearance with the use of a special solution.
What to Expect
Both procedures are considered minimally invasive and require only local anesthetics. To prepare you, here’s how they are done:
- Ambulatory Phlebectomy. Small incisions are made by our specialists with the use of special tools and a vein hook. Done under local anesthetics, vein removal can take about an hour. Compression stockings will be used after the treatment to improve healing.
- Injection Sclerotherapy. A fine needle with a special solution will be inserted in the small blood vessels. This will cause the varicose veins to shrink. Our specialists will determine how many injections are needed for the treatment. Special stockings are also worn after the procedure to facilitate healing.
Interested in these venous procedures? Contact us to discuss your symptoms and the best varicose vein treatment options for you!