
Prescott’s Leading Group of Subspecialty Radiologists
Vascular Specialists and Interventional Radiologists Provide Specialized Care for Prescott’s Community
About Vascular and Interventional Specialists of Prescott
Vascular & Interventional Specialists of Prescott (VISP) has been a part of the Prescott medical community and serving patients since 2010. We are a group of subspecialty radiologists that perform numerous minimally-invasive, low-risk procedures using the tools of our trade for guidance—x-ray, ultrasound, CT scan, and MRI. Our goal is to educate the public and medical community, then diagnose and treat people in the safest, most compassionate way, with rapid recovery times and low risk of complications.
Meet Our Doctors
The physicians at VISP offer a vast background and thorough experience in diagnostic and interventional radiology, specializing in minimally invasive procedures using image guidance. The subspecialty group also provides therapeutic treatment through specific procedures to help alleviate chronic and severe back pain.
Click here to learn more about the specialties of Dr. Dicker, Dr. Lloyd, and Dr. Paxton.
Procedures
- Back – VISP offers an array of therapies to treat chronic and severe back pain such as caudal epidurals, nerve block procedures, sciatica epidurals, injections similar to a cortisone injection, and vertebral cement augmentation.
- Arterial – The physicians at VISP are vascular specialists who work with patients with peripheral vascular disease (PVD) or peripheral arterial disease (PAD) to provide treatments to correct narrowed or blocked vessels to ease blood circulation throughout the body.
- Vein – Patients will see our varicose vein specialists for top-level care to treat uncomfortable and painful varicose veins, spider veins and reticular veins. Vein ablation procedures are nonsurgical and provide a quick recovery time.
- Cancer – The interventional specialists at VISP perform specific cancer therapy treatments to help shrink the size of tumors in cancer patients. Learn more here about the types of therapies offered.
- Epidurals – An epidural injection is a method to deliver pain-relieving and anti-inflammatory medicine to the epidural layer of the spine. VISP physicians use epidurals often to relieve severe back pain and chronic back pain in their patients.
- Nerve Blocks – Nerve block injections are used to alleviate pain by way of turning off the pain signal to the brain. The doctors at VISP use the nerve block procedure often in patients who are experiencing debilitating pain in their bodies. Learn more about the procedure here.
- Other – There are many procedures that we do at VISP with precision and care including implanting MediPorts, J Tube Placements, PICC Lines, IVC Filter Placement and Removal, Biopsies, and more.
Conditions We Treat
The hardworking and diligent team of physicians at VISP performs an array of diagnostic testing, procedures and treatment options for many conditions. Area physicians often refer to us because we are well-known and trusted to provide the best in care for our patients who are experiencing the following:
Latest News

Cryoablation for Cancer Treatment: Your Ultimate Guide
Did you know that cryoablation, a less invasive and innovative therapy, is gaining popularity as a cancer treatment option? In this comprehensive guide, we will walk you through everything you need to know about cryoablation and its potential as an effective treatment for cancer. From understanding its mechanism of action to exploring its benefits and applications, we have got you covered. Understanding Cryoablation in Oncology At VISP, we strive to provide comprehensive information about cryoablation in oncology. Cryoablation is a minimally invasive procedure commonly performed by skilled interventional radiologists who specialize in minimally invasive procedures. This innovative therapy offers a promising treatment option for cancer patients, harnessing the power of extreme cold temperatures to destroy cancer cells. The Cryoablation Procedure During the cryoablation procedure, a probe guided by imaging techniques such as ultrasound or CT scan is inserted into the tumor. This allows for precise placement of the probe and accurate visualization of the tumor. The tumor is then targeted and frozen using extreme cold temperatures, leading to the destruction of cancer cells. Throughout the cryoablation procedure, careful monitoring and control of the freezing process ensure precision and efficacy. This precision is crucial to minimize damage to surrounding healthy tissues and maximize the effectiveness of the treatment. Mechanism of Action Cryoablation works by inducing cell death in cancer cells through freezing. When the tumor is subjected to extreme cold temperatures, ice crystals form within the cancer cells, causing cellular damage and ultimately leading to their death. This process, known as apoptosis, triggers the body’s immune response, aiding in the elimination of cancer cells. Additionally, cryoablation promotes an anti-tumor immune response, which can potentially target and destroy any remaining cancer cells, further enhancing the effectiveness of the treatment. Understanding the cryoablation procedure and its mechanism of action provides valuable insights into the unique benefits and potential of this innovative therapy. In the next section, we will compare cryoablation to other cancer treatments, exploring what sets it apart and why it may be the preferred choice in certain cases. Comparing Cryoablation to Other Cancer Treatments When considering cancer treatments, it’s important to explore all available options. Cryoablation, a minimally invasive procedure, offers distinct advantages over traditional treatments such as surgery, radiation, and chemotherapy. Understanding what sets cryoablation apart and why it may be the right choice for certain patients is crucial in making informed treatment decisions. What Sets Cryoablation Apart? Cryoablation stands out for its minimally invasive nature, which involves small incisions and shorter recovery times compared to surgery. This makes it an appealing option for patients seeking a less invasive treatment approach. Additionally, cryoablation has fewer side effects compared to radiation and chemotherapy, preserving quality of life during treatment. Its precise targeting capabilities are another key advantage, ensuring that only the cancerous cells are affected while sparing healthy tissue. Why Choose Cryoablation? For certain patients, cryoablation may be the preferred treatment choice. If a tumor is located in a sensitive area where surgery may be risky, cryoablation provides a safer alternative. Moreover, patients who are unable to tolerate radiation therapy due to medical conditions can benefit from cryoablation’s versatility. The procedure can also effectively treat multiple tumors located in different areas of the body, providing a comprehensive treatment option for patients with various tumor locations. Additionally, cryoablation can be repeated if necessary, allowing for ongoing treatment as needed. The Role of Cryoablation in Cancer Treatment Cryoablation plays a significant role in cancer treatment as both a primary therapy and a palliative treatment. As a primary therapy, cryoablation can be used to treat small tumors or as an alternative to surgery, radiation, or chemotherapy. This innovative technique utilizes extreme cold temperatures to destroy cancer cells, offering a less invasive option for patients. With cryoablation, patients can experience shorter recovery times and fewer side effects compared to traditional treatments. In palliative treatment, cryoablation is used to relieve symptoms and improve the quality of life for patients with advanced cancer. It can effectively control pain and bleeding associated with tumors, providing much-needed relief. Cryoablation offers a promising approach to managing advanced cancer and enhancing patients’ well-being. Whether used as a primary therapy or a palliative treatment, cryoablation provides patients with an additional option in their cancer treatment journey. Its versatility and effectiveness make it a valuable tool in the hands of skilled medical professionals. At our facility, our team of experts is dedicated to utilizing cryoablation to its fullest potential and providing comprehensive care to our patients. Conclusion Cryoablation offers an innovative and effective approach to cancer treatment. Its minimally invasive nature and ability to minimize side effects make it an attractive option for many patients. We are proud to be at the forefront of this revolutionary therapy, continuously striving to provide the best care possible. As technology advances and more research is conducted, cryoablation is expected to have an even greater impact on cancer treatment. The ongoing development in this field holds the potential for improved outcomes and expanded applications. At VISP, we remain committed to staying abreast of these advancements to offer our patients the latest and most effective treatment options available. If you have any further questions or are interested in exploring cryoablation as a potential treatment option, don’t hesitate to contact us. Our dedicated team is here to provide you with the information and support you need to make informed decisions about your healthcare. Contact us today to learn more about cryoablation and discover if it is the right treatment option for you.
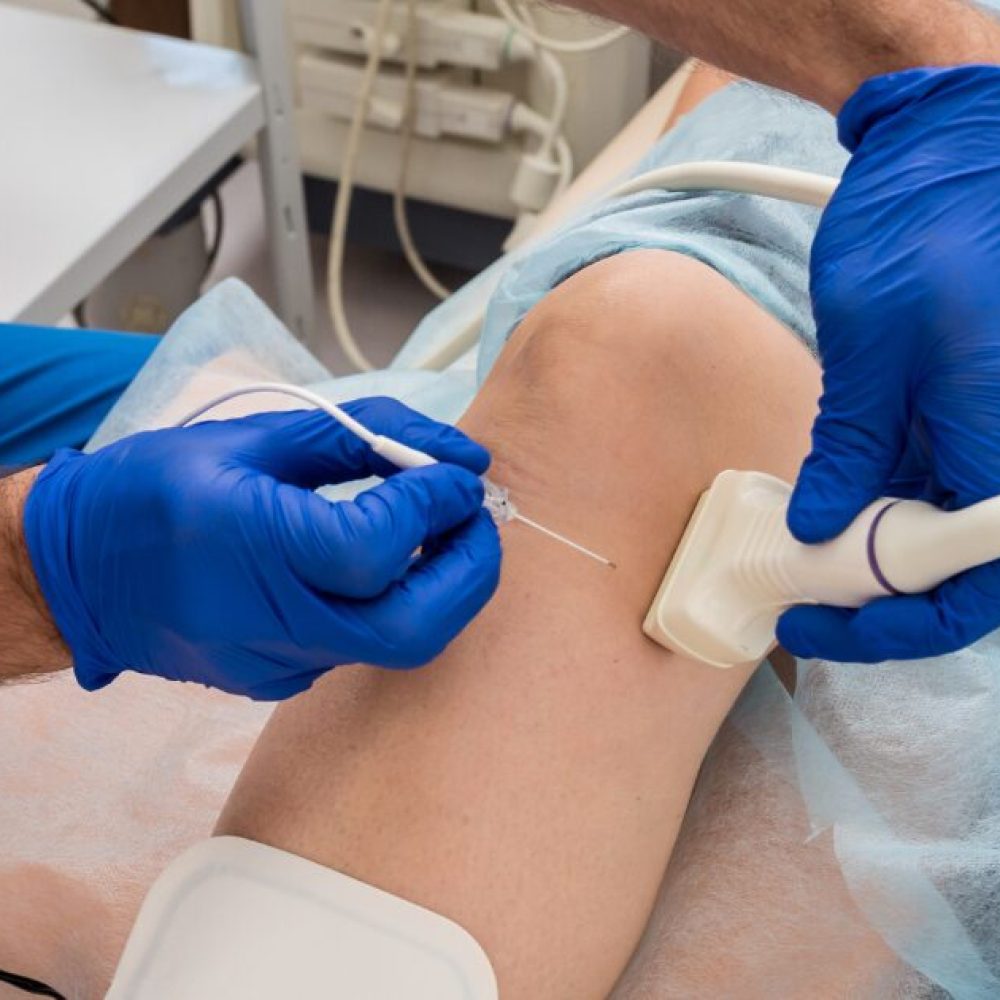
What Is Radiofrequency Ablation Procedure?
In the dynamic landscape of medical advancements, minimally invasive procedures are increasingly becoming the forefront of pain management across various medical disciplines. Among these innovative techniques lies Radiofrequency Ablation (RFA). In this comprehensive guide, we will delve into what RFA entails, how it is performed, the reasons behind its use, and the associated benefits. What is the Radiofrequency Ablation Procedure? Radiofrequency ablation (RFA), is a medical procedure used to treat conditions such as chronic pain, certain cancers, and abnormal heart rhythms (arrhythmias). The technique employs high-frequency electrical currents to generate heat within targeted tissues, thereby eliminating abnormal cells or nerves responsible for pain or irregular heartbeats. By using radiofrequency energy, a physician can precisely target specific tissues and block their ability to send pain signals without causing extensive damage to surrounding areas. Who is a Good Candidate for Radiofrequency Ablation? Determining a patient’s suitability for Radiofrequency Ablation (RFA) involves evaluating several factors, including their medical condition, symptoms, treatment history, and overall health. While the specific criteria may vary depending on the medical indication for RFA, here are some general characteristics that often make a patient a good candidate for the procedure: Chronic Pain Conditions Patients experiencing conditions originating from the spine, such as neck pain, joint pain, chronic low back pain, knee pain, pelvic concerns, and peripheral nerve pain, are often good candidates for RFA. It is also used to treat arm and leg pain. These individuals may have failed to achieve adequate relief with conservative treatments such as pain medication, physical therapy, or steroid injections. Imaging-Confirmed Lesions Patients with identifiable lesions or abnormalities on diagnostic imaging studies, such as X-rays, MRI scans, CT scans, or ultrasound, may be suitable candidates for RFA. The presence of well-defined target tissues or tumors that can be visualized and accurately localized on imaging facilitates the precise placement of the radiofrequency probe during the procedure. [Related: What Causes Tumors? (Guide to Benign & Malignant Tumors)] Failed Conservative Treatments Patients who have undergone conservative treatments without significant improvement in symptoms or functional limitations may benefit from RFA. The procedure offers an alternative or adjunctive therapeutic option for individuals who have exhausted non-invasive interventions and continue to experience persistent pain or disability. Limited Surgical Options Patients who are poor candidates for traditional surgical interventions due to underlying medical conditions, advanced age, or surgical risk factors may find RFA to be a viable treatment alternative. RFA’s minimally invasive nature and reduced procedural risks make it particularly attractive for individuals who may not tolerate extensive surgery or anesthesia. Localized Tumors or Lesions Patients with localized tumors or lesions that are amenable to thermal ablation may benefit from RFA as a curative or palliative treatment option. RFA is commonly used in the management of primary and metastatic tumors affecting organs such as the liver, lungs, kidneys, bones, and soft tissues. Desire for Minimally Invasive Treatment Patients who prefer minimally invasive treatment approaches and wish to avoid the potential risks, complications, and prolonged recovery associated with open surgery may opt for RFA. The procedure offers a shorter recovery time, reduced postoperative pain, and fewer cosmetic concerns compared to traditional surgical interventions. Realistic Treatment Expectations Patients who have realistic expectations regarding the outcomes, limitations, and potential risks of RFA are more likely to be satisfied with the procedure. Healthcare providers should engage in open and transparent communication with patients, discussing the anticipated benefits, possible side effects, and expected recovery timeline associated with RFA. How It’s Done The radiofrequency ablation procedure is typically performed in an outpatient setting. The key steps include the following: 1. Patient Evaluation and Preparation Before undergoing RFA, patients undergo a comprehensive evaluation by their healthcare provider. This evaluation includes a review of medical history, physical examination, and diagnostic imaging studies such as X-rays, MRI, or CT scans. Patients may be advised to discontinue certain medications or refrain from eating and drinking for a specific period before the procedure. 2. Anesthesia Administration The RFA procedure typically requires numbing medication such as local anesthesia to numb the area where the catheter or probe will be inserted. In some cases, sedation may also be administered to help patients remain comfortable and relaxed during the procedure. 3. Imaging Guidance To ensure accurate placement of the RFA probe, imaging guidance techniques such as fluoroscopy, ultrasound, or CT scans are utilized. These imaging modalities allow the healthcare provider to visualize the target tissue in real time and guide the catheter or probe to the precise location. 4. Catheter or Probe Insertion Once the target area is identified under imaging guidance, the healthcare provider inserts a thin, flexible catheter or probe through the skin and into the target tissue. The insertion site is often numbed with a local anesthetic to minimize discomfort. 5. Confirmation of Placement After the catheter or probe is inserted, its placement is confirmed using imaging techniques. The healthcare provider ensures that the catheter or probe is positioned accurately within the target tissue, allowing for optimal delivery of radiofrequency energy. 6. Radiofrequency Energy Delivery: Once the catheter or probe is correctly positioned, radiofrequency energy is delivered through the device. The radiofrequency energy heats the targeted tissue, causing thermal ablation and destruction of the problematic cells or nerves. The duration and intensity of the energy delivery may vary depending on the specific condition being treated and the size of the target area. 7. Monitoring and Adjustment Throughout the RFA procedure, the healthcare provider monitors the patient’s vital signs and adjusts the energy delivery as needed to ensure safe and effective treatment. Continuous monitoring helps to minimize the risk of complications and ensures optimal outcomes. 8. Post-Procedure Care After the RFA procedure is completed, patients are monitored for a short period in a recovery area to ensure their stability. In most cases, patients can return home on the same day. They receive instructions on post-procedure care, including recommendations for pain management, activity restrictions, and follow-up appointments. 9. Follow-Up and Monitoring Following RFA, patients undergo regular follow-up appointments with their healthcare provider to assess treatment outcomes and monitor for any signs of recurrence or complications. Additional imaging studies may be performed to evaluate the effectiveness of the procedure and track changes in the target tissue over time. Reasons Why It’s Done Chronic Pain Management: RFA is commonly used to treat chronic pain conditions such as arthritis, back pain, and nerve pain by disrupting pain signals. Cancer Treatment: In oncology, RFA destroys tumors in the liver, kidneys, lungs, and bones, especially for patients who are not candidates for surgery. Cardiac Arrhythmias: RFA can correct abnormal heart rhythms by targeting and destroying abnormal electrical pathways in the heart tissue. Benefits of Radiofrequency Ablation Procedure Minimally Invasive Procedure As a minimally invasive procedure, radiofrequency ablation offers patients an alternative to traditional open surgeries. Unlike conventional surgical procedures, RFA typically involves small incisions, reducing trauma to surrounding tissues and minimizing postoperative pain. The use of local anesthesia further enhances patient comfort during the procedure. Preservation of Healthy Tissue One of the primary advantages of RFA is its ability to precisely target and destroy diseased tissue while preserving adjacent healthy structures. This targeted approach minimizes collateral damage, reduces the risk of complications, and enhances the overall safety profile of the procedure. By sparing healthy tissue, RFA contributes to faster recovery times and improved patient outcomes. Customized Treatment Options RFA offers healthcare providers a high degree of flexibility in tailoring treatment plans to meet individual patient needs. The procedure can be adapted to address a wide range of medical conditions across various anatomical sites, including the spine, liver, lungs, kidneys, and cardiac tissue. This versatility makes RFA a valuable therapeutic tool in the management of diverse clinical scenarios, from chronic pain syndromes to cancerous tumors. Outpatient Procedure and Reduced Hospitalization In many cases, RFA can be performed on an outpatient basis, allowing patients to return home on the same day of the procedure. This outpatient approach offers several advantages, including reduced healthcare costs, minimized disruption to daily routines, and enhanced patient convenience. By avoiding prolonged hospital stays, RFA enables patients to resume their normal activities more quickly, promoting a faster return to functional independence. Effective Chronic Pain Management Chronic pain conditions, such as facet joint pain, sacroiliac joint dysfunction, and neuropathic pain syndromes, can significantly impair quality of life and functional capacity. RFA serves as an effective pain management strategy by disrupting pain signals transmitted by dysfunctional nerve pathways. By ablating the sensory nerves responsible for transmitting pain signals, RFA provides successful pain relief and improves patient comfort, facilitating greater mobility and engagement in daily activities. Complementary Therapy and Multimodal Approach RFA can be integrated into comprehensive treatment plans as part of a multimodal approach to patient care. It may complement other therapeutic modalities, including pharmacological interventions, physical therapy, and interventional procedures, to achieve synergistic effects and optimize treatment outcomes. By addressing multiple aspects of a patient’s condition, RFA enhances the overall efficacy of the treatment regimen and promotes holistic healing. Minimal Downtime and Rapid Recovery Compared to traditional surgical procedures, RFA typically involves minimal downtime and rapid recovery. Most patients experience only mild discomfort or soreness following the procedure, which can be effectively managed with over-the-counter pain medications. With proper post-procedural care and guidance, patients can resume their usual activities and gradually increase their level of physical exertion as tolerated. Answers to Common Questions How painful is radiofrequency ablation? Radiofrequency ablation is generally well-tolerated. Patients may experience mild discomfort, but local anesthesia and sedation are often used to minimize pain during the procedure. Post-procedural discomfort is usually manageable with over-the-counter pain medications. How long does it take to recover from radiofrequency ablation? Patients typically experience mild discomfort or cramping for a few days post-procedure. Recovery is generally quick, with patients resuming normal activities within a few days to a week. Individual recovery experiences may depend on the specific condition being treated and the patient’s overall health. What are the disadvantages of radiofrequency ablation? While RFA is generally considered safe, like any medical procedure, it may carry some risks, including infection, bleeding, temporary discomfort, or damage to surrounding structures. It may not be suitable for all patients, and individual responses vary. Patients should discuss potential risks and benefits with their healthcare provider before undergoing the procedure. Consult With VISP Today Radiofrequency Ablation stands as a remarkable advancement in medical science, offering targeted and minimally invasive solutions for a spectrum of conditions. From chronic pain management to oncological interventions and cardiac care, the versatility of RFA is a testament to its efficacy. As individuals and healthcare practitioners explore the potential of radiofrequency ablation, it is imperative to make informed decisions. Consulting with a qualified healthcare provider is the first step toward understanding how this procedure can address specific health concerns. VISP provides comprehensive care and expertise in the field of interventional radiology, including radiofrequency ablation procedures. Our team of vein doctors and interventional radiologists is dedicated to delivering personalized, patient-centered care, tailored to meet individual needs and preferences. Schedule a consultation with our experts today and take the first step towards improved health and well-being.
What Are the Signs a Nerve Block Is Wearing Off?
Nerve blocks serve as invaluable tools in modern medicine, offering targeted pain relief for a variety of conditions, ranging from postoperative pain control to chronic pain management. Understanding the signs a nerve block is wearing off is crucial for effective patient care and management. In this comprehensive guide, we will explore what nerve blocks entail, elucidate the signs signaling their waning efficacy, and address common questions surrounding their duration and management. Understanding Nerve Blocks Nerve blocks are medical procedures involving the injection of numbing medication, usually a local anesthetic, near specific nerves to alleviate pain temporarily. It works by temporarily interrupting the transmission of pain signals along the nerves. These blocks play a crucial role in pain management for various conditions, including surgical procedures and chronic pain. Depending on the type of nerve block administered and the medications used, the duration of pain relief can vary significantly. Types of Nerve Blocks Nerve blocks can be categorized based on their target location and the purpose of the intervention. Some common types include: Peripheral Nerve Blocks (Peripheral Nerve Blockade): These blocks involve the injection of local anesthetics near peripheral nerves located outside the central nervous system. A peripheral nerve block can target specific regions of the body, such as the arms, legs, abdomen, and face. Examples include brachial plexus blocks for upper extremity procedures and femoral nerve blocks for lower extremity surgeries. Epidural and Spinal Blocks: Administered near the spinal cord, these blocks are commonly used for pain relief during childbirth, certain surgeries, or to manage chronic pain conditions. Sympathetic Nerve Blocks: Targeting the sympathetic nervous system, these blocks are employed to manage pain conditions like complex regional pain syndrome (CRPS) and certain vascular disorders. Facet Joint Blocks: Applied to the facet joints of the spine, these blocks are utilized for diagnostic purposes and to alleviate pain arising from these joints. Intercostal Nerve Blocks: Targeting the nerves along the ribcage, these blocks are often employed for postoperative pain management or to alleviate pain associated with conditions like shingles. Understanding the specific type of nerve block administered is crucial in predicting the expected duration of pain relief and recognizing potential signs of its wearing off. [Related: The Different Types of Nerve Blocks] Signs a Nerve Block Is Wearing Off Despite their effectiveness, nerve blocks are not permanent solutions. Recognizing when a nerve block is wearing off is crucial for ensuring timely intervention and maintaining optimal pain management. Here are key signs to watch for: 1. Return of Sensation Patients may experience the return of sensation in the affected area, signaling the fading effectiveness of the nerve block. You may begin to notice a resurgence of pain, tingling, or discomfort as the anesthetic effects diminish. 2. Increasing Pain Levels As the nerve block wears off, pain levels typically rise. This escalation often occurs gradually but may become more pronounced over time. 3. Decreased Duration of Pain Relief You might observe that the duration of pain relief provided by the nerve block becomes shorter over time. This diminishing effect signals the wearing off of the block and necessitates attention. 4. Difficulty Resuming Normal Activities As the nerve block weakens, you may experience discomfort or pain upon movement. This is particularly noticeable in the context of postoperative pain relief and management when the patient resumes normal activities that were previously manageable. 5. Temperature Changes Sensitivity to temperature variations in the affected area may increase as the nerve block loses its efficacy. You may notice heightened sensitivity to hot or cold stimuli. 6. Muscle Weakness or Tremors Muscle weakness or trembling can be indicative of a diminishing nerve block. As the nerve signals regain strength, muscle control may be compromised. 7. Gradual Return of Motor Function Depending on the type of nerve block, the return of motor function in the affected area can be a clear sign that the block is wearing off. You may regain the ability to move fingers, toes, or other body parts. Addressing Common Questions What’s the longest a nerve block can last? The duration of a nerve block varies depending on several factors, including the following: type of block administered specific medications used concentration of the pain medication individual patient characteristics While some nerve blocks may provide relief for several hours, others can last for days or even weeks. For instance, anesthetic nerve blocks for hand surgery normally last 6-8 hours, whereas nerve blocks for pain management following total knee replacement can last 12-24 hours. When should you seek medical attention after a nerve block? Seek medical attention if you experience severe or persistent pain, swelling, redness, or other concerning symptoms following a nerve block. Additionally, any signs of infection or adverse reactions necessitate prompt evaluation by a healthcare professional. How long does it take for a nerve block in the arm to wear off? The duration of a nerve block in the arm can vary depending on the specific type of block performed and the medications utilized. In general, peripheral nerve blocks in the arm may provide pain relief for several hours to a few days before gradually wearing off. Proactive Management Tips for Patients After undergoing a nerve block procedure, it’s important for patients to take an active role in managing their recovery and monitoring for signs that the nerve block is wearing off. Here are some proactive tips to help you navigate this process effectively: Monitor Your Symptoms: Keep a close eye on any changes in sensation or pain levels in the treated area. Note the gradual return of feeling, tingling, or discomfort, as these could be indicators that the nerve block is wearing off. Follow Your Doctor’s Instructions: Your healthcare provider will provide you with post-procedure instructions. Adhering to these guidelines is essential for a successful recovery. These instructions may include information on managing pain, recommended activities, and when to seek medical attention. Effective Communication: Establish open communication with your healthcare team. Don’t hesitate to report any concerns or changes in your symptoms promptly. Your feedback is invaluable in guiding the healthcare provider to make any necessary adjustments to your pain management plan as your nerve block wears off. Keep a Pain Journal: Consider maintaining a pain journal to track your daily experiences. Record the intensity and nature of your pain, as well as any activities that seem to impact it positively or negatively. This journal can be a valuable tool during follow-up appointments to refine your pain management plan. Understand Your Pain Management Plan: Work collaboratively with your healthcare team to develop a comprehensive pain management plan. This plan may include a combination of nerve blocks, medications, physical therapy, and other interventions tailored to your specific needs. Set Realistic Expectations: Recognize that the effectiveness of a nerve block may vary, and the duration of pain relief is not uniform for everyone. Setting realistic expectations allows you to better navigate the transition from the relief provided by the nerve block to managing any returning sensations. Stay Positive and Patient: Recovery is a gradual process. Stay positive and be patient with yourself as you navigate through the phases of post-procedural recovery. Celebrate small victories, and don’t hesitate to reach out to your healthcare team for support and guidance. Take the Next Step Towards Pain Relief Understanding the signs a nerve block is wearing off empowers patients and healthcare providers to proactively manage pain and ensure optimal outcomes. Timely recognition of these signs enables appropriate interventions, promoting a seamless transition in pain management strategies. If you’re experiencing persistent discomfort or considering nerve block therapy, schedule a consultation with VISP today. Our experienced team is dedicated to guiding you towards effective solutions for your vascular and pain management needs. Don’t let pain compromise your quality of life. Contact VISP and begin your path to relief today.
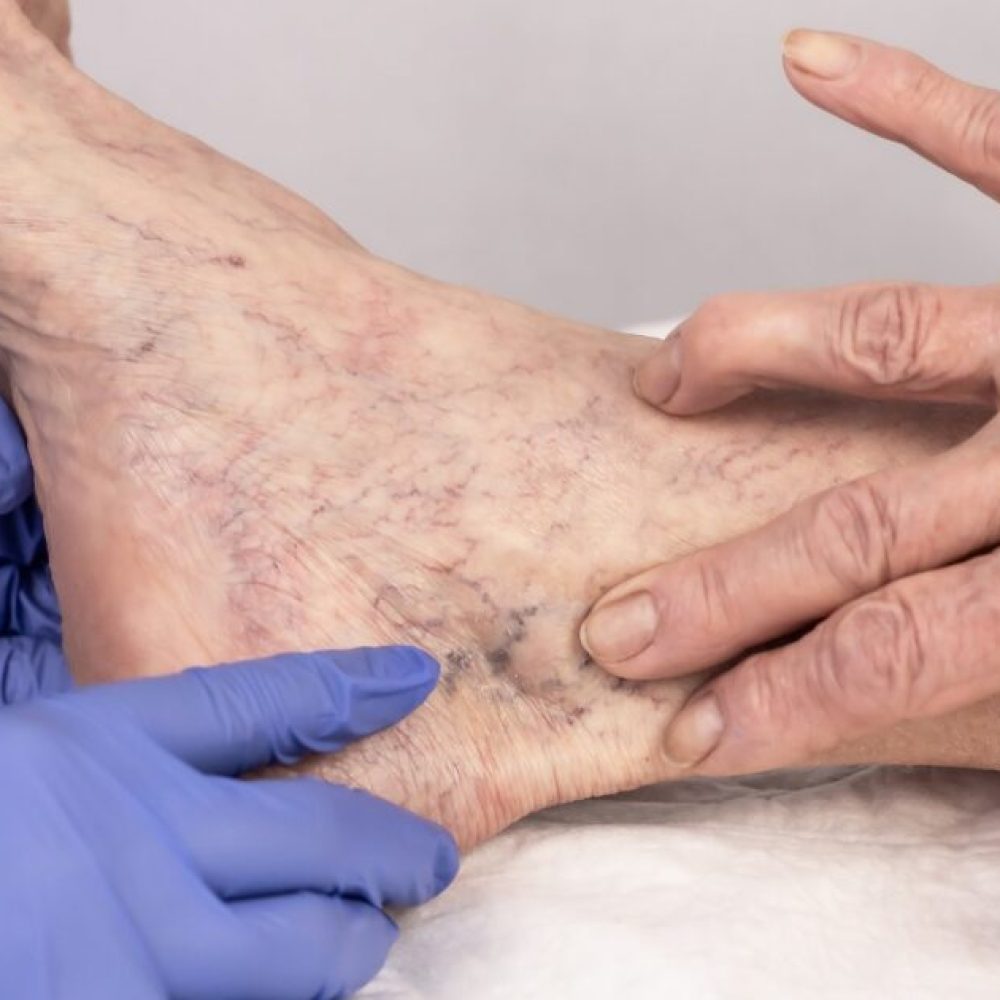
How Long Does Sclerotherapy Last?
Spider and varicose veins not only affect one’s appearance but can also lead to discomfort and health concerns. Sclerotherapy, a widely embraced medical procedure, offers an effective solution. This minimally invasive procedure involves injecting a solution directly into affected veins, prompting them to collapse and gradually fade away. In this comprehensive guide, we delve into the intricacies of sclerotherapy, shedding light on not just the procedure itself but also the critical question: How long does sclerotherapy last? Keep reading below to learn more. What is Sclerotherapy Treatment? Sclerotherapy involves the injection of a specialized solution directly into affected veins, inducing their collapse and subsequent fading. This minimally invasive treatment has gained immense popularity for its dual benefits—addressing both aesthetic concerns and providing relief. Ideal Candidates Candidates for sclerotherapy typically include individuals with varicose veins, spider veins, or other vascular concerns. Sclerotherapy may not be suitable for: Breastfeeding Mothers: Due to potential risks, breastfeeding individuals are generally advised against undergoing sclerotherapy. Pregnant Women: It is recommended to wait at least three months after delivery before considering Sclerotherapy. Those with Superficial or Deep Vein Thrombosis: Individuals with either superficial or deep vein thrombosis may not be suitable candidates for Sclerotherapy. Patients under Bed Rest: Sclerotherapy requires some level of mobility for optimal results. Patients confined to bed rest may not be suitable candidates. Birth Control Users: In most cases, individuals on birth control can undergo the procedure unless contraindicated by their primary care physician. However, considerations may vary based on individual health circumstances. History of Blood Clots: Eligibility depends on the nature and severity of past blood clots. Individuals with a history of blood clots should discuss their case with a healthcare professional to determine suitability. Individuals considering sclerotherapy are encouraged to consult with a vein specialist. A thorough examination and discussion of medical history can help determine the most suitable treatment approach. The Procedure in Detail Consultation and Assessment Before undergoing sclerotherapy, a thorough consultation and assessment are conducted to determine the severity of the vein issue and the most suitable treatment plan. Preparation The patient is often advised to avoid certain medications and activities in the days leading up to the procedure. This ensures optimal conditions for the treatment. The Injection Process During the procedure, a fine needle is used to inject the sclerosing solution directly into the targeted veins. Patients may experience a mild discomfort or a stinging sensation. Post-Procedure Care After the injections, patients are usually instructed to wear compression stockings to promote proper blood circulation and healthy veins, as well as enhance the effectiveness of the treatment. [Related: 9 Things to Ask Your Varicose Vein Doctor About Your Treatment] How Long Does Sclerotherapy Last? The duration of sclerotherapy varies among individuals. Typically, patients begin witnessing improvements within weeks to months after the procedure. However, several factors can influence the longevity of its effects: 1. Size and Severity of Varicose Veins The size and severity of the veins being treated play a role in determining the number of sessions required, thereby influencing the overall treatment duration. Larger veins or more advanced cases might necessitate additional sessions, extending the overall treatment duration. 2. Individual Healing Response Each individual’s body heals at a unique pace. Consequently, the rate at which veins disappear post-sclerotherapy can differ. 3. Post-Procedure Care Adherence to recommended post-procedure care is instrumental in ensuring optimal and lasting results. Your doctor will most likely recommend that you wear compression stockings, maintain an active lifestyle, and avoid prolonged periods of sitting or standing to improve your blood flow. Make sure to follow your doctor’s post-procedure instructions for safer and faster recovery. [Related: Sclerotherapy Aftercare: Dos and Don’ts] Frequently Asked Questions 1. What is the Downside of Sclerotherapy? While sclerotherapy is generally safe, patients may experience mild side effects. These can include redness, bruising, or itching at the injection site. In rare cases, complications such as blood clots or allergic reactions may occur. It’s crucial to discuss potential risks and benefits with your healthcare provider before undergoing the procedure. 2. How Often Do You Need Sclerotherapy? The frequency of sclerotherapy sessions varies. While some patients achieve desired results after one or two treatments, others with more complex cases may require additional sessions. The interval between sessions allows for proper healing and assessment of the treatment’s effectiveness. 3. Do Veins Grow Back After Sclerotherapy? Sclerotherapy has a high success rate in treating existing veins, but it doesn’t guarantee the permanent prevention of new varicose veins. While treated veins generally do not grow back, new ones may develop over time. Maintaining a healthy lifestyle, including regular exercise and proper leg elevation, can contribute to preventing new vein problems. 4. What is the Success Rate of Sclerotherapy? Research indicates promising primary and secondary success rates at 36 months for treated veins using sclerotherapy. The majority of patients experience significant improvement in both the cosmetic appearance of their legs and the relief of symptoms associated with varicose or spider veins. Additional Considerations 1. Preparing for Sclerotherapy Before undergoing sclerotherapy, patients should communicate any medical conditions, medications, or allergies to their healthcare provider. A comprehensive assessment ensures a safe and effective procedure. 2. Combining Sclerotherapy with Other Treatments In certain cases, combining sclerotherapy with other treatments such as laser therapy or ambulatory phlebectomy may enhance results. A personalized approach is key to addressing individual needs comprehensively. 3. Potential Risks and Complications While sclerotherapy is generally safe, it’s essential to be aware of potential risks and complications, including infection, ulceration, or changes in skin pigmentation. Open communication with your healthcare provider is crucial to address any concerns. 4. Lifestyle Modifications In addition to the procedural aspects, incorporating healthy lifestyle habits can contribute to the overall success of sclerotherapy. Maintaining a healthy weight, avoiding prolonged periods of sitting or standing, and wearing compression stockings as recommended by your healthcare provider are essential aspects of post-sclerotherapy care to improve blood flow and your overall condition. Consulting a Trusted Vein Doctor Is the Way to Go Sclerotherapy stands as an effective and minimally invasive solution for those grappling with varicose and spider veins. Understanding the factors influencing its duration is crucial for informed decision-making. While it offers a high success rate, it’s essential to consider individual variations and follow recommended post-procedure care for optimal results. By consulting with a qualified vein specialist, adhering to post-treatment guidelines, and making necessary lifestyle modifications, individuals can experience lasting relief and improved leg aesthetics. Sclerotherapy not only addresses the visible signs of problematic veins but also contributes to enhancing overall vascular health. Schedule Your Consultation Today! If you are considering sclerotherapy and wish to explore how it can benefit you, schedule a consultation with Vascular & Interventional Specialists of Prescott (VISP). Our experienced team is dedicated to providing personalized care, guiding you through the process, and helping you achieve the best possible results. Don’t wait—take the first step towards healthier, more beautiful legs.

Nerve Block Pros and Cons: A Comprehensive Overview
Curious about a pain relief option that doesn’t involve surgery? Nerve blocks have emerged as a valuable tool in addressing stubborn body pain, and this guide aims to provide a thorough understanding of their applications, benefits, and potential drawbacks. Whether you’re considering this option or just exploring pain management alternatives, it’s essential to fully understand nerve block pros and cons. Keep reading below to learn more! What Is Nerve Block Procedure? A nerve block, or peripheral nerve blockade, is a minimally invasive treatment where a nerve-numbing substance is injected to manage or prevent various types of intractable pain. This technique aims to disrupt pain signals between the nerves and the brain, offering a potential way to alleviate discomfort. Who Are the Candidates for a Nerve Block Procedure? Individuals experiencing nerve pain persisting for three months, who have explored conservative treatments like physical therapy, over-the-counter pain relievers, and prescription medications (such as gabapentin, pregabalin, or duloxetine), may find relief through interventional nerve treatments like nerve blocks. Nerve blocks offer a targeted approach to pain management, aiming to disrupt pain signals and provide effective relief for those who have exhausted traditional avenues of treatment. This procedure aims to enhance the overall quality of life by increasing functionality in daily activities, such as work, exercise, and routine tasks. Types of Nerve Blocks: Cervical Nerve Blocks: Purpose: Identify and alleviate neck, shoulder, or arm pain by targeting the cervical spine. Procedure: Steroid injections are utilized to reduce inflammation, promoting the healing of damaged nerves for both diagnostic and long-term pain relief. Thoracic Nerve Blocks: Purpose: Address pain in the mid-back region, chest, and abdomen. Procedure: Identify the specific nerve causing pain in the targeted area, allowing for a precise treatment plan. Numbing medication can be injected for temporary or longer-term pain relief. Lumbar Nerve Blocks: Purpose: Identify and relieve pain originating from the lower back and legs (sciatica). Procedure: Immediate pain relief can be achieved, and if the initial nerve block is successful, a series of treatments may be scheduled for longer-term relief. Intercostal Nerve Blocks: Purpose: Identify the source of pain in and around the ribs. Procedure: Useful for those experiencing rib pain, requiring a chest tube insertion, or seeking relief from pain due to rib fractures. This procedure serves both diagnostic and therapeutic purposes. Peripheral Nerve Blocks: Purpose: Manage pain in specific body regions, such as the face (trigeminal nerve block) or limbs. Procedure: Peripheral nerve block involves the injection of an anesthetic near a peripheral nerve. These nerve block options offer a tailored approach to pain management, allowing our patients to pinpoint the source of their discomfort and receive targeted relief. If you find yourself dealing with persistent pain in specific areas, exploring these nerve block options could be a valuable step toward a more comfortable and active life. Note: Always consult with your healthcare professional to determine the most suitable treatment plan for your individual needs. [Read more: The Different Types of Nerve Blocks] Nerve Block Pros and Cons Pros Effective Pain Management: Nerve blocks offer swift and almost immediate relief from pain, providing patients with an efficient solution for their discomfort. Minimized Use of Pain Medications: By targeting the source of pain directly, nerve blocks can reduce reliance on traditional pain medications, minimizing potential side effects associated with long-term drug use. Temporary Pain Relief for Chronic Conditions: Individuals suffering from chronic pain conditions can benefit from temporary relief through nerve blocks, allowing them to experience periods of comfort. Reduced Need for Surgery: In certain cases, nerve blocks can diminish the necessity for invasive surgical procedures, offering a less intrusive alternative for pain management. Improved Functionality: Nerve blocks can enhance overall functionality, enabling patients to engage in daily activities, work, and exercise more comfortably. [alt text: nerve block procedure] Cons Temporary Relief: One of the drawbacks of nerve blocks is that their effects are not permanent. Multiple procedures may be required to sustain prolonged relief. Potential Side Effects and Risks: While generally safe, nerve blocks may result in side effects such as numbness, weakness, or allergic reactions. These effects are typically temporary. Complications may include rare occurrences of nerve damage, infection, bleeding, or allergic reactions, but our highly trained medical professionals prioritize safety and take precautions to minimize these risks. Discomfort During Injection: While the procedure is generally well-tolerated, some patients may experience temporary discomfort or pain during the injection. This can be managed with local anesthesia or sedating medicine administered before the procedure. What Can Go Wrong With a Nerve Block? Nerve blocks are generally considered safe, with complications being rare. Our highly trained medical professionals prioritize safety and take precautions to minimize risks. While there may be temporary discomfort during the injection, this can be effectively managed with local anesthesia or sedation administered before the procedure. Always consult with our experienced healthcare professionals to understand the potential benefits and risks based on your health profile. Is a Nerve Block Worth It? Deciding on a nerve block depends on your pain management goals, the nature of your condition, and consultation with a healthcare professional. How Many Years Does a Nerve Block Last? Generally, nerve blocks can provide temporary pain relief that may last anywhere from a few hours to several days. The duration of relief varies among individuals. Nerve blocks may offer temporary relief, and the need for repeat procedures depends on the case. Tired of Chronic Pain? Get a Medical Consultation Today! Nerve blocks present a promising option for pain management, offering effective relief with minimal invasiveness. Whether you’ve endured chronic pain in the neck, back, or limbs, or sought relief from rib-related discomfort, the tailored approach of nerve blocks may be your key to a more comfortable and active life. If you resonate with the challenges discussed in this guide and believe nerve blocks might be the right path for you, we encourage you to take the next step.Schedule a consultation with VISP today. Let us collaborate to understand your unique pain management needs and explore how nerve blocks can be integrated into your personalized treatment plan. Regain control over your life and embark on a journey toward effective, targeted pain relief.

What Is A Nerve Block Procedure?
Did you know that 20.4% of adults in the USA have chronic pain? This pain can impact every aspect of your life, and traditional pain management methods may not always be effective. That’s where nerve block procedures come in. A nerve block procedure is a type of pain management procedure that involves injecting a local anesthetic to temporarily block the transmission of pain signals along the nerves. At its core, nerve blocks fall under the umbrella of pain management, aimed at alleviating discomfort and improving the overall quality of life. Keep reading to learn more about the details of nerve block procedures and how they can help you manage your pain. Taking a Closer Look at Nerve Blocks When it comes to managing pain caused by various medical conditions, nerve blocks are becoming an increasingly popular option for temporary pain relief. Nerve blocks involve injecting local anesthetic medications into a group of nerves that are responsible for causing pain in a specific area of the body. The Different Types of Nerve Blocks Nerve blocks are medical interventions used to control or manage pain by blocking the transmission of nerve signals to relieve pain. They can be classified into surgical and non-surgical methods, each with its own applications and considerations. Surgical Nerve Blocks: Surgical Sympathectomy: Involves cutting or damaging specific nerves to disrupt the sympathetic nervous system. Applications: Used for conditions like complex regional pain syndrome (CRPS) or excessive sweating (hyperhidrosis). Neurectomy: Procedure: Surgical removal or transection of a nerve. Applications: May be performed to treat certain types of chronic pain when other treatments have failed. Peripheral Nerve Decompression: Procedure: Surgical decompression of nerves from entrapment or compression. Applications: Often employed for conditions like carpal tunnel syndrome or cubital tunnel syndrome. Spinal Cord Stimulation (SCS): Procedure: Implantation of electrodes near the spinal cord, delivering electrical impulses to disrupt pain signals. Applications: Used for chronic pain conditions, including failed back surgery syndrome and complex regional pain syndrome. Non-surgical Nerve Blocks: Local Anesthetic Injections: Procedure: Involves injecting a local anesthetic near a nerve or group of nerves. Applications: Commonly used for diagnostic purposes to identify the source of pain or for therapeutic pain relief. Epidural Steroid Injections: Procedure: Injection of a corticosteroid and anesthetic into the epidural space around the spinal cord. Applications: Often used for pain management in conditions such as herniated discs or spinal stenosis. Facet Joint Injections: Procedure: Injection of anesthetic and/or corticosteroid into the facet joints of the spine. Applications: Used for pain relief in conditions affecting the facet joints, such as arthritis. Peripheral Nerve Blocks: Procedure: Injection of anesthetic near a peripheral nerve. Applications: Used to manage pain in specific regions of the body, such as the face (trigeminal nerve block) or limbs. Radiofrequency Ablation (RFA): Procedure: Application of radiofrequency energy to a nerve to create a heat lesion, disrupting pain signals. Applications: Commonly used for chronic pain conditions, particularly in the spine. How Nerve Blocks Work When we experience pain, it’s usually caused by a specific group of nerves in the affected area. Nerve blocks work by targeting this specific group of nerves and stopping the pain signal from reaching the brain. This is achieved by injecting a local anesthetic medication into the area around the affected nerves, which numbs the area and provides pain relief. The Different Types of Nerve Blocks We Offer There are many types of nerve blocks, each targeting a specific group of nerves. Some of the most common nerve blocks that we offer include: Nerve Block TypeDescriptionCervical Nerve BlocksInvolve the injection of anesthetic or anti-inflammatory medication around nerves in the cervical (neck) region. These blocks are often used to diagnose and manage pain stemming from issues such as cervical disc herniation, arthritis, or nerve compression.Thoracic Nerve BlocksTargets the nerves in the thoracic (mid-back) region. By injecting medications near these nerves, often using fluoroscopic guidance, healthcare providers aim to alleviate pain associated with conditions like thoracic spine fractures, intercostal neuralgia, or post-herpetic neuralgia.Lumbar Nerve BlocksInvolve the injection of medications around the nerves in the lumbar (lower back) region. These blocks are commonly employed for diagnostic purposes to identify the source of lower back pain or as therapeutic interventions for conditions such as lumbar disc herniation or facet joint arthritis.Intercostal Nerve BlocksTarget the nerves running between the ribs. By injecting local anesthetics or steroids near these nerves, healthcare providers can provide pain relief for conditions like shingles (herpes zoster) affecting the intercostal nerves or post-surgical pain following thoracic surgeries. The Nerve Block Injection Procedure The nerve block injection procedure involves injecting a local anesthetic medication around the affected nerves, which usually takes only a few minutes to complete. In some cases, a nerve catheter may be used to deliver medication continuously to the affected area. This is done by inserting a tiny plastic tube into the area around the nerves, which can be left in place for several days. Benefits of Nerve Blocks Nerve blocks offer many benefits for managing pain caused by various medical conditions. Some of the key benefits include: Providing immediate pain relief Minimizing the use of pain medications Providing temporary pain relief for chronic pain sufferers Reducing the need for surgery in some cases Safety and Efficacy of Nerve Blocks First and foremost, nerve blocks are generally considered safe. Complications are rare, but as with any medical procedure, they can occur. Risks associated with nerve blocks include: Nerve damage Infection Bleeding Allergic reactions However, our highly trained and experienced medical professionals take every precaution to minimize these risks. While nerve blocks are generally safe, it is important to note that they can cause temporary discomfort or pain during the injection. However, this discomfort can be managed with the use of local anesthesia or a sedating medicine, which are administered to patients prior to the procedure. Nerve Blocks vs. Other Treatment Methods When it comes to treating pain, there are different treatment methods available, including nerve blocks. Nerve blocks provide the advantage of medication continuously delivered to the affected area, which can help manage pain for longer periods compared to other methods where the effect wears off after a few hours. Unlike other methods that provide generalized pain relief, nerve blocks target specific nerves responsible for causing pain. By targeting specific nerves, nerve blocks are more precise and effective in treating certain conditions, including chronic pain. Nerve blocks are typically performed in an operating room, and the procedure itself can take a few hours to complete. However, the duration of pain relief depends on the specific type of block performed. Treatment MethodsAdvantagesDisadvantagesMedication Continuously Delivered– Provides longer-lasting pain relief- Can be tailored to individual needs– May require catheter insertion- Risk of infectionNerve Blocks– Precise and effective in targeting specific nerves- Can be used to diagnose and treat pain– May require multiple injections- Risk of adverse effects like nerve damageOral Medications– Easy to administer- Available over-the-counter– Effect is not long-lasting- May cause side effects like stomach upset As with any medical procedure, there are risks associated with nerve blocks, such as the possibility of nerve damage or adverse reactions to medication. However, these risks can be mitigated by consulting with a trusted medical provider specializing in pain management, like VISP. At VISP, we believe in a patient-centered approach to pain management where we work with our patients to develop a personalized treatment plan. Contact us today to learn more about how we can help manage your pain. Start a Pain Free Life Today! At VISP, we understand the importance of pain management and the impact it has on the daily lives of individuals. That’s why we offer nerve block procedures as a solution to help provide temporary pain relief. By targeting specific nerves and using local anesthetics, we can help alleviate the discomfort associated with various conditions. We aim to make the process as comfortable as possible for our patients, providing them with the care and attention they deserve. Through nerve block procedures, we can help manage pain caused by nerve cells affected by various medical conditions. We advocate for temporary pain relief, and our goal is to improve our patients’ quality of life. Contact us today to learn more about nerve block procedures and how we can help you achieve pain relief and management. FAQ What is a nerve block procedure? A nerve block procedure is a medical technique used to achieve temporary pain relief. It involves injecting a local anesthetic near a specific group of nerves responsible for causing pain. How do nerve blocks work? Nerve blocks work by targeting a specific group of nerves that transmit pain signals. By blocking the transmission of these signals, nerve blocks can provide temporary pain relief. What are the different types of nerve blocks? There are various types of nerve blocks commonly used in medical practice. Some examples include occipital nerve blocks, celiac plexus blocks, and stellate ganglion blocks. What does the nerve block procedure involve? The nerve block procedure may involve injecting a local anesthetic near the affected nerve or using a nerve catheter. In some cases, a tiny plastic tube may be used to deliver the anesthetic. How do nerve blocks provide pain relief? Nerve blocks provide pain relief by delivering a numbing medication to the affected area. This numbs the nerves and temporarily blocks the pain signals from being transmitted to the brain. Are nerve blocks safe? Nerve blocks are generally considered safe when performed by trained medical professionals. Safety measures are taken to minimize risks, and potential side effects are carefully monitored. How do nerve blocks compare to other treatment methods? Nerve blocks offer advantages such as continuous pain relief compared to other methods where the effect wears off after a few hours. They specifically target the nerves causing pain and can be performed in an operating room. What are the benefits of nerve block procedures? Nerve block procedures provide temporary pain relief, improving the quality of life for individuals suffering from various conditions. To learn more about the benefits of nerve block procedures, you can contact VISP, a trusted medical provider specializing in pain management.

