The Top 3 Warning Signs of DVT (Deep Vein Thrombosis)

Deep vein thrombosis (DVT) is a condition that occurs when a blood clot (thrombosis) forms in one or more veins of your body, usually in the legs. Although it is a treatable condition, it can be serious and life-threatening if not treated early.
According to healthcare research, around 600,000 individuals are affected by DVT annually in the United States.
Knowing the early and warning signs is essential to alleviate this growing number of cases and to save more lives.
Read this article to know more about DVT.
What causes DVT?
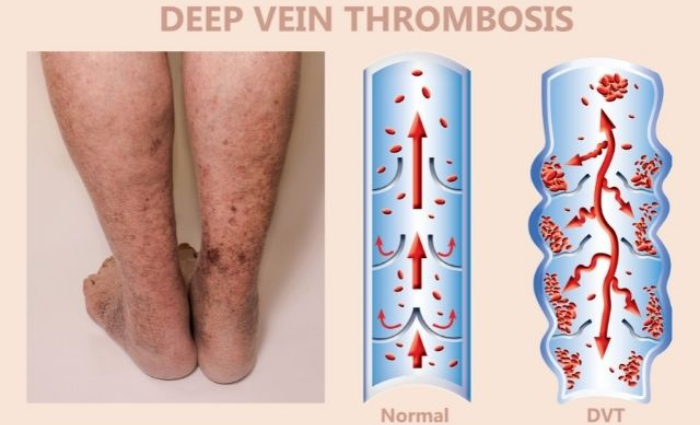
Blood clot formation can occur anytime and to anyone but people with underlying medical conditions that affect their blood supply are more prone to DVT.
Deep vein thrombosis (DVT) occurs when blood flow slows down in the deep veins of the body and often goes unnoticed until the patient feels pain or there is a noticeable swelling. The blood clot forms and blocks the vein which prevents the blood from properly circulating, leading to severe pain.
Anything that blocks the proper flow of blood may cause clots that result in DVT.
The main causes of blood clots are injury or damage to the blood vessels, surgery, trauma, or infection. Many factors trigger these causes, including:
- Old age
- Personal or family history of blood clotting disorders or DVT or pulmonary embolism
Varicose veins and other leg vein diseases - Vein injuries from muscle inflammation, trauma, fractures, or surgery in the abdomen and lower body
- Smoking
- Being overweight or obese
- Recent major surgery
- Cancer and chronic medical conditions involving internal organs
- Poor blood circulation due to prolonged bed rest, limited lower body movement, or paralysis
- Hormone therapy or birth control pills
- Pregnancy
- Having a Central Venous Catheter (CVC)
- Rare genetic conditions that affect blood clotting factors
It is important to detect DVT at an early stage and watch out for warning signs to prevent serious manifestation and disability.
Signs and Symptoms of Deep Vein Thrombosis
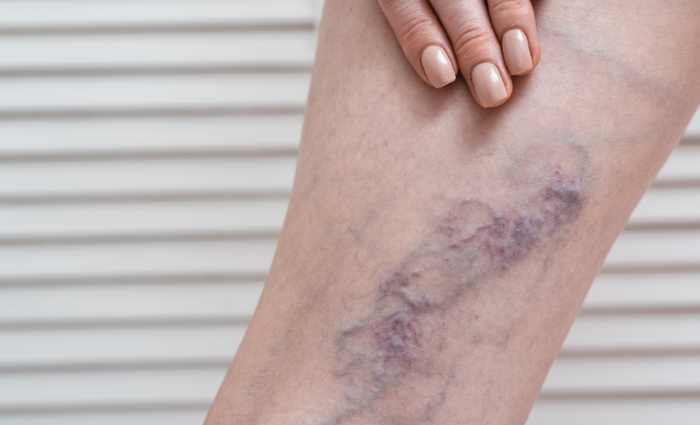
DVT can be a fatal condition if left untreated but curable when you start noticing the early signs of a blood clot.
The common and early blood clot symptoms that lead to DVT include:
- Swelling of the affected area
- Leg pain
- Reddish, bluish, or pale skin around the affected leg
- Throbbing or cramping pain
[Read: 5 SIGNS OF DEEP VEIN THROMBOSIS]
Top Warning Signs of DVT and Pulmonary Embolism
How serious can deep vein thrombosis get?
A report from the Center for Disease Control and Prevention shows that 10-30% of DVT patients will die within a month after being diagnosed.
Apparently, many people don’t recognize the early symptoms and fail to seek medical treatment before their condition becomes serious. About 25% of DVT patients experience sudden death from pulmonary embolism, one of its most life-threatening complications.
Pulmonary embolism, a potentially fatal medical condition, occurs when a blood clot travels through your circulation system. It can block blood flow to your lungs and cause blood vessel damage, particularly to your pulmonary arteries.
Recognizing the warning signs of deep vessel thrombosis or pulmonary embolism is crucial.
These are the top symptoms that you need to keep an eye on:
- Sudden shortness of breath. Breathing difficulties that intensify with exertion
- Unexplained, sharp, and tight chest pain. It can feel like you are having a heart attack. You can feel it when you cough, bend or stoop.
- Coughs with blood.
Other warning signs of PE associated with DVT include:
- Painful shoulder, back, jaw, or arm
- Lightheadedness, dizziness, or worse, fainting
- Fast, irregular heartbeat
- Rapid pulse
One-third to one-half of DVT patients will experience long-term complications (postthrombotic syndrome), which include swelling, pain, scaling, and discoloration in their affected limbs.
DVT/PE is responsible for between 60,000 to 100,000 deaths in the United States. If you have any of the abovementioned symptoms, call 911 immediately or go to an emergency room for immediate medical attention.
How to prevent blood clots?
Like any other illness, preventing DVT starts with maintaining an active and healthy lifestyle. Sitting and standing for long periods should be avoided altogether.
Additionally, smoking and dehydration are among the risk factors of blood clots. Avoiding or quitting smoking and drinking enough water daily will help maintain good blood flow, and eventually, prevent DVT.
For people with a family history of deep venous thrombosis and pulmonary embolism, having regular checkups to monitor symptoms and prevent future clots is extremely recommended.
[For more DVT prevention tips, read: HOW TO PREVENT DVT (5 TIPS FROM A VEIN SPECIALIST)]
How To Treat DVT?
Your doctor may recommend these treatments depending on the results of your blood tests and diagnostic tests:
Anticoagulant (blood thinners)
The doctor will prescribe anticoagulation medication (blood thinners) once the case has been confirmed by a blood test. These medications prevent blood clots from happening again and dissolve any existing ones.
If blood-thinning medications are taken in large doses, they can cause excessive bleeding. A doctor should strictly supervise the use of these medications for DVT.
Regular blood tests may be done to determine how long it takes for blood to clot. This is to allow your doctor to prescribe the right dosage of anticoagulants.
Compression stockings
Compression stockings give a tight squeeze at the lower leg up to the knee where it slightly loosens.
Wearing compression stockings is a non-invasive way of treating DVT and reducing discomfort. Compression stockings help reduce the swelling and the chance of developing more clots.
Inferior Vena Cava (IVC) Filter Placement
In cases where the patient will not be able or is not allowed to take blood thinners, placement of an Inferior Vena Cava filter may be suggested to prevent pulmonary embolism. This filter will be placed inside the large abdominal vein or the inferior vena cava which supplies blood to the heart.
Installing the filter will be done by inserting a metal device into the abdominal vein. This IVC filter will extricate any clot and will prevent it from reaching the heart or lungs.
However, the usage of the IVC filter is limited only for some time. It will just be a substitute until the patient can ingest blood thinners and anticoagulants.
DVT surgery
For severe cases which can no longer be treated with medications and other non-invasive treatments, surgery will be required.
Performing surgery to remove clots has a lot of risks, such as infections and excessive bleeding. It is not recommended by most doctors unless severe complications arise like tissue damage.
[For an in-depth discussion of DVT treatment options, read: HOW TO TREAT DEEP VEIN THROMBOSIS? HERE’S A DEFINITIVE GUIDE]
When to consult a doctor
Deep vein thrombosis should be talked with a health professional the moment it is suspected to prevent it from getting more serious. Those who had deep vein thrombosis should still consult their doctor since there are cases where patients developed recurrent blood clots.
If you think you’re at risk of deep vein thrombosis and pulmonary embolism, book your appointment with a vein specialist.
Vascular & Interventional Specialists of Prescott was formed in 2010 by a group of subspecialty radiologists that perform numerous minimally-invasive, low-risk procedures using the tools of our trade for guidance—x-ray, ultrasound, CT scan, and MRI. The team’s goal is to educate patients and medical communities, while also providing safe and compassionate health care, with rapid recovery times and low risk of complications.
